Ventilation and airflow are especially important in operating rooms for controlling thermo-hygrometric conditions, providing gas removal, diluting airborne contamination and minimizing bacteria transfer airborne. Each and every one of these considerations has certain requirements that must be met, in order to maintain a safe and comfortable environment for patients and staff.
These requirements include aspects such as thermal comfort, control of the concentration of pollutants (i.e., bacteria and viruses), and room temperature regulation. Depending on the nature of the operating room environment, even extremely specific factors such as air velocity at the patient wound location needing to be below a threshold value of 0.2 m/s must be acknowledged.
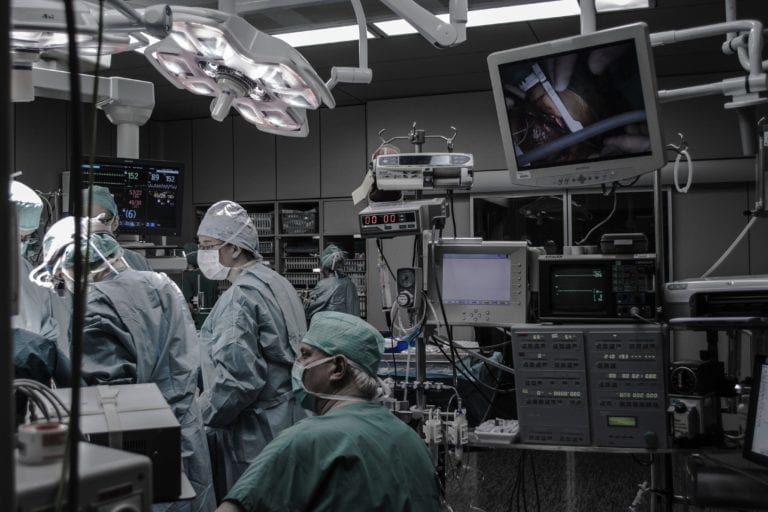
All of these aspects are controlled by the ventilation strategy implemented in the given room. Therefore, for these requirements to be met efficiently, design engineers must count on analysis tools that provide the most reliable and detailed information as possible. In this blog post, we have provided a case study using computational fluid dynamics (CFD) to analyze and optimize the ventilation system of a hospital operating room.
Learn how to use fluid flow simulation to test and optimize the ventilation of hospitals and other healthcare environments.
Applications of CFD in Hospitals
The use of CFD in the planning of ventilation systems provides design engineers with many advantages. The use of simulation allows them to solve the flow problem with a computer, obtaining precise results, and model the case with varying grades of geometry simplification. This, in turn, optimizes computation time and resources, allowing engineers to calculate the temperature at every point in the geometry, as well as calculate the magnitude and direction of the velocities. This ability allows engineers to then predict the movement of bacteria and contaminants on a granular level via three-dimensional information.
Some of the common goals achieved by engineers with CFD analysis of airflow include:
- Optimizing air movements in closed spaces by eliminating air recirculation zones
- Saving energy through more efficient heating and/or cooling
- Reducing the spreading of bacteria by removing airborne bacteria through effective ventilation
- Improving thermal comfort levels for patients and medical staff
- Quickly regulating temperature without large overshoots.
The advantages and benefits of CFD have turned it into a very popular tool for closed space ventilation, such as hospitals rooms.
Case Study: Airflow in an Operating Room
The case study detailed below was kindly provided by Veryst Engineering and was presented by Alireza Kermani, Ph.D. P.E., Senior Engineer at Veryst Engineering, in this joint webinar.
Our case study model consists of a typical hospital operating room. This includes simplified geometries for patient and doctor, bed, wardrobe, hospital equipment, illumination, and ventilation:
-
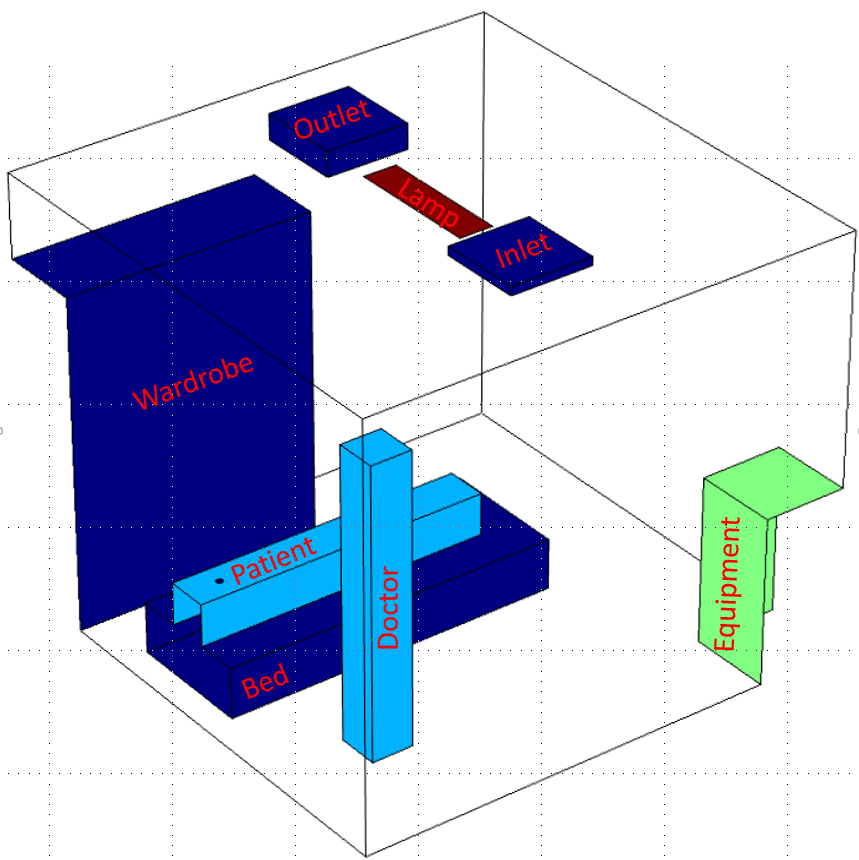
Model of a hospital operating room
In this case study, the floor, walls, and ceiling are considered to be heat insulated. The ventilation flow rate is based on an estimate of 6 ACH (air changes per hour) and the typical air inlet temperature. Thermal loads are used for bodies, equipment, and illumination:
-
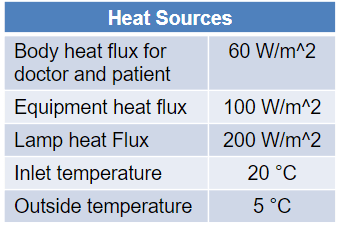
Thermal loads and boundary condition
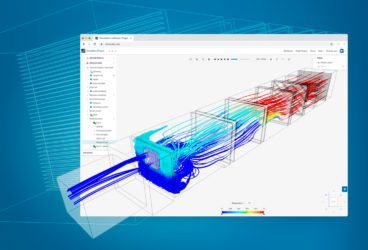
The following image is a visualization of air flow results from the CFD simulation of the operating room:
-
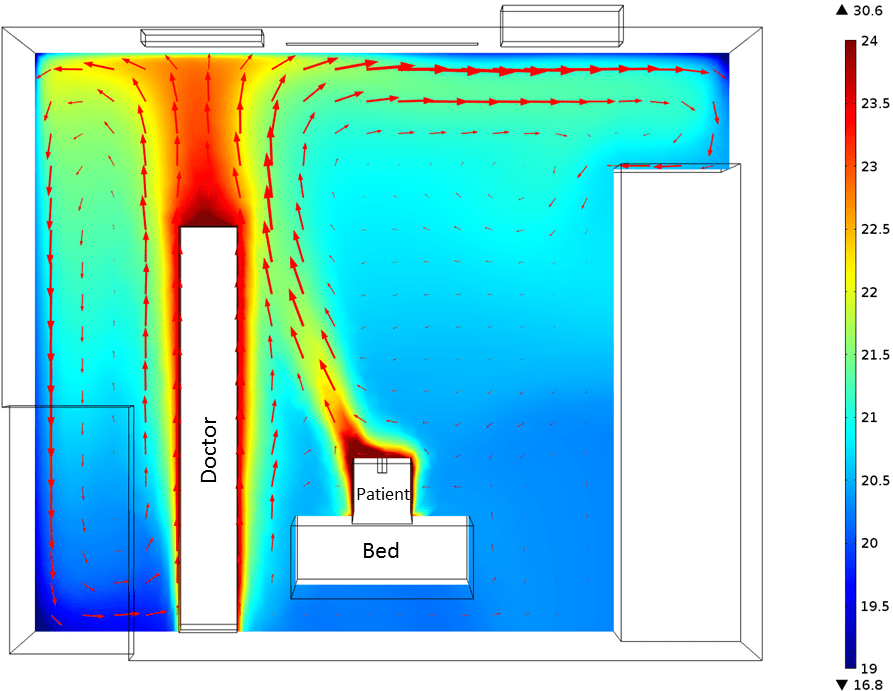
Results of the airflow simulation of the hospital operating room. Color scale corresponds to air temperature in °C.
CFD Simulation Findings
In our case study, it was found that a recirculation zone occurred behind the doctor. This outcome was not desired, as bacteria and other contaminants could get trapped in this area. The fluid flow simulation also found that there was a flow of air from the patient towards the doctor, which also needed to be reconfigured in the design. Another recirculation zone was discovered above the wardrobe, which again could have resulted in airborne bacteria concentration. The flow at the wound site of the patient was also examined in order to see that the velocity threshold value requirement was met.
-
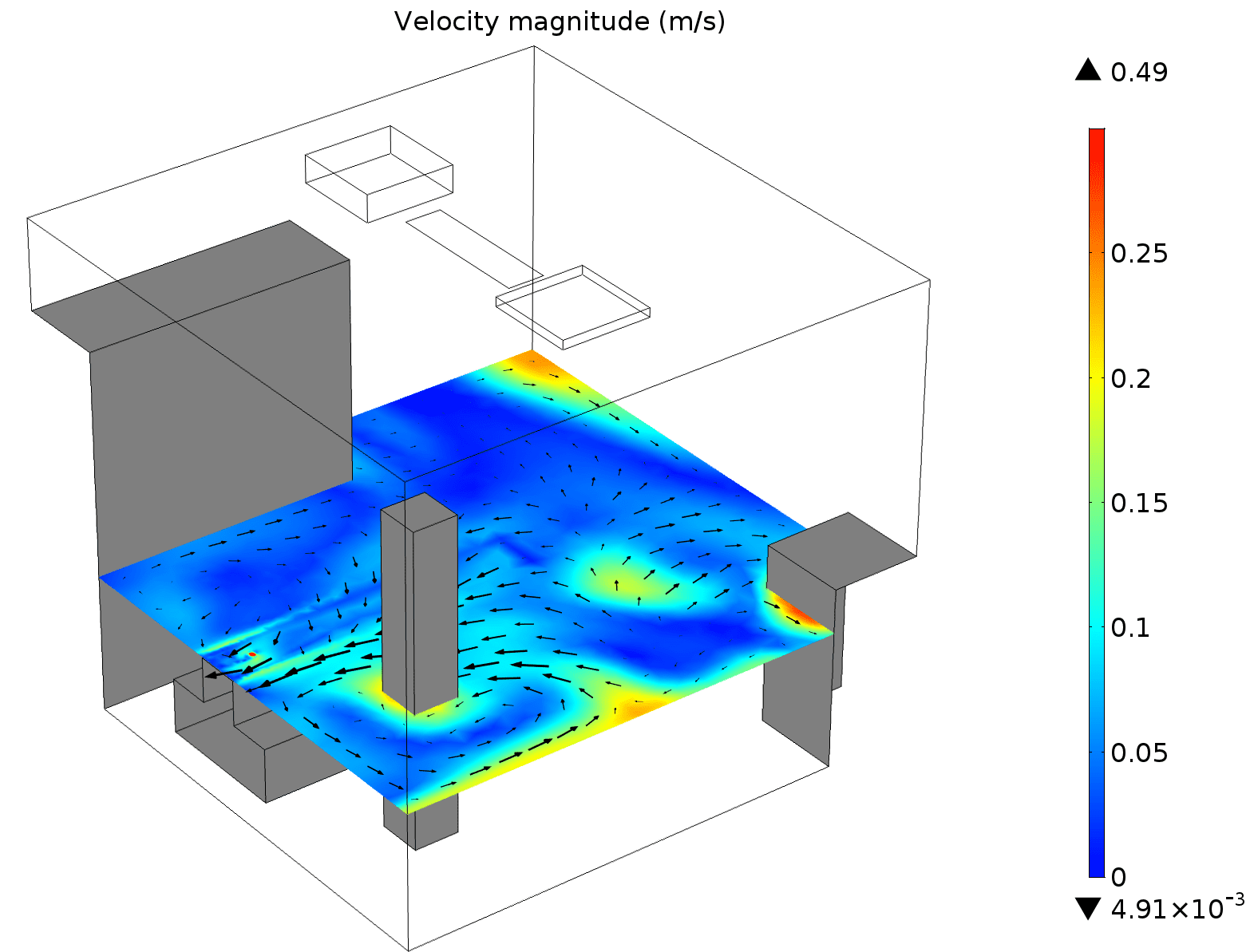
Airflow velocity at wound level. Color corresponds to flow velocity magnitude in m/s.
Thermal Comfort in the Hospital Operating Room
In cases like these, thermal comfort is a relative criterion as it controls the satisfaction of occupants within the environment. This factor is not directly related to the equations of flow but instead assessed by subjective evaluation. One technique used by engineers is to correlate the results of registered psychological experiments as published in standards with thermal analysis variables, such as flow temperature, velocity, and humidity, which can be obtained from CFD analysis results.
The results for the test case showed that there is a probability of 56% that the patient is dissatisfied with the room temperature, with an overall sensation of being cold.
Airborne Transmission of Bacteria
In our case study, airborne transmission due to coughing was also analyzed. After coughing, the portion of large droplets fall on the floor, and the portion of smaller droplets become aerosolized and start to move with the airflow. The change of airflow due to coughing is modeled using experimental data for cough flow rate vs. time. The following bacteria movement pattern was found:
-

Airborne bacteria spreading due to coughing. Color corresponds to air flow velocity in m/s.
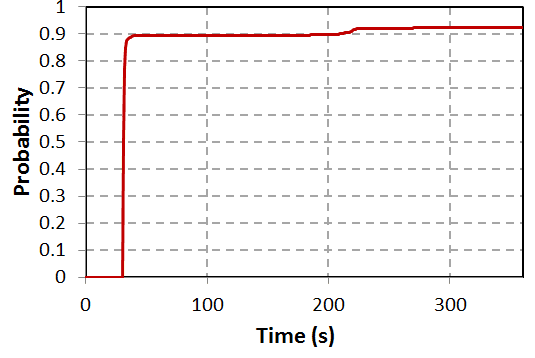
It can be seen that most of the bacteria leave the room through the ventilation exhaust 30 seconds after coughing occurs. Yet, due to flow recirculations, some of the bacteria remains in the room, which is not desired. The following plot shows the percentage of bacteria that leaves the room at the ventilation outlet versus time, which correlates with the probability of infection:
We see that 90% of the bacteria leave the room at around the 30 seconds mark, but even after 360 seconds, the remaining 10% of the bacteria stays inside the room and is never picked up by the ventilation exhaust system. This poses a problem.
Design Optimization for the Operating Room Ventilation
The chief question that arises from this situation is: how can we use this information to improve the ventilation system so bacteria is removed faster and thermal comfort is improved? One possible method is to move the location of the ventilation exhaust, by leaving all other design variables untouched. After examining the flow pattern, three design alternatives were proposed:
-
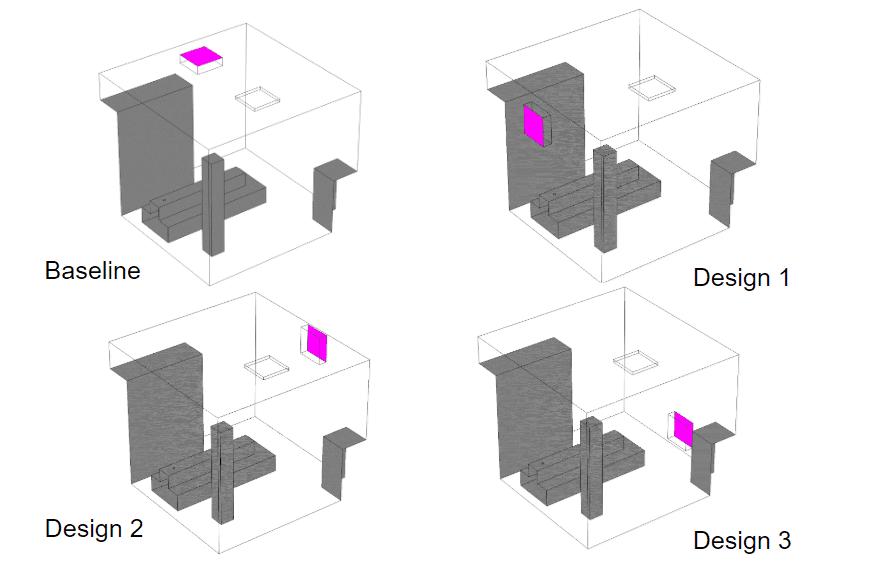
Design candidates for airflow optimization. Pink faces show the location of the ventilation outlet.
All three design variations are modeled and simulated with CFD. Here is the comparison of the airflow pattern results among the design variations:
-
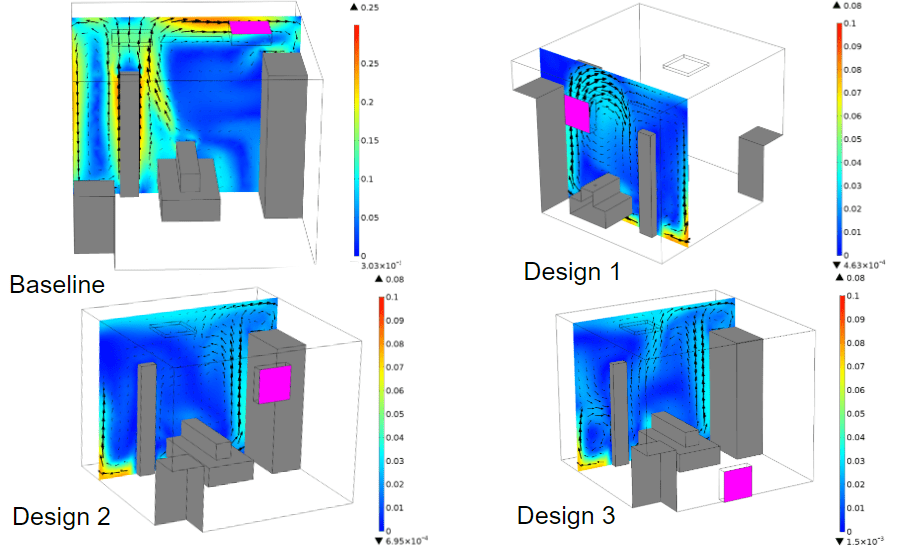
Simulation results comparison for design candidates. Color legend corresponds to flow velocity magnitude in m/s.
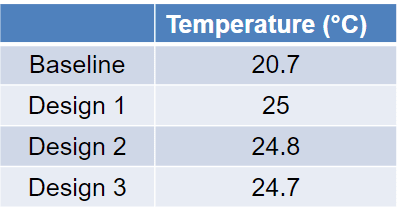
In design 1, a recirculation zone exists above the patient, but with low velocities in the plane. The next design (Design 2) there is only a minor recirculation next to the wardrobe. In the final design, (design 3) there is a recirculation zone behind the doctor, at a low level. We also compare the average temperature of the room for each design. We find that the energy efficiency can only be improved by relocating the ventilation outlet:
In order to compare airborne transmission of bacteria performance for the various ventilation strategies, this plot is used to show the bacteria leaving the room through the ventilation exhaust in time:
-
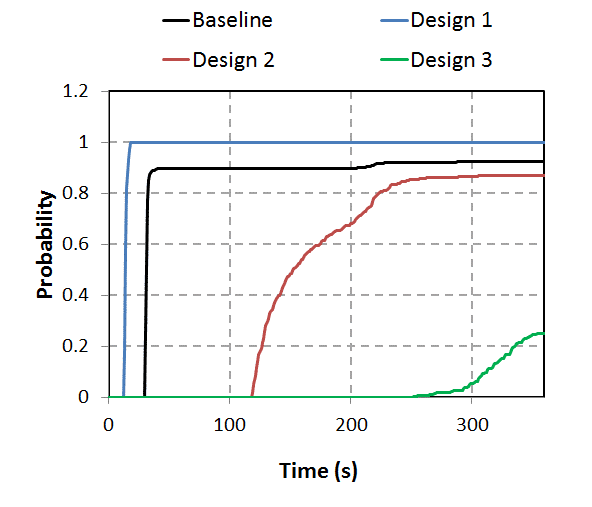
Percentage of bacteria leaving the room through the ventilation exhaust. Comparison of design versions.
We see that design 1 removes all bacteria at around 15 seconds. This design corresponds with the air outlet located above the head of the patient. The other designs actually perform worse than the original configuration.
Conclusion
Through our case study, it was shown that the airflow of an operating room can be optimized with CFD simulation. CFD has many benefits including:
- Increasing comfort levels and improving ventilation design and energy efficiency of buildings
- Gaining better insight into aerosol contamination dispersion characteristics to optimize airflow pattern in hospitals, laboratories and cleanrooms.
A great way to begin leveraging CFD technology is with the SimScale platform, which can be accessed online, via a standard web browser. To discover how to start your own airflow simulation, check out our public projects.